What Causes Fingernails to Turn Yellow?
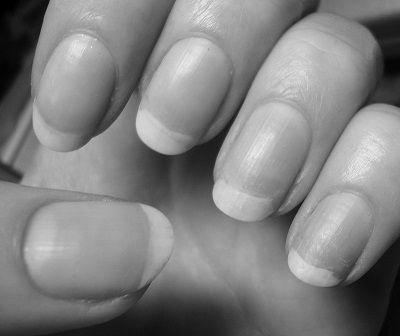
If you’ve ever wondered, “What causes fingernails to turn yellow?” you’re not alone. Fungus, a fungal infection, or genetics may all be contributing factors. But which one is yours? And how do you treat it? Read on for answers! Listed below are some possible causes of yellowing fingernails. Also, read on for tips on treating this inherited condition.
Onycholysis

Onycholysis can be challenging to diagnose. If you notice that the yellow color of your fingernails is persistent and affects more than one digit, you may need to see a dermatologist. The condition is not an emergency, but if you continue to have symptoms, it may signify a more serious underlying condition. Fortunately, onycholysis is treatable, and the state will usually clear up on its own in a few months.
Onycholysis is caused by a condition in which the nail plate separates from the nail bed, exposing the white tissue underneath. This causes the fingernail to turn yellow and thicken. Treatment for this condition depends on the type of fungus, which can be treated with prescription or topical antifungal medication. In some cases, a fungal infection in the fingernails can be treated by applying a topical or oral antifungal medication.
Onycholysis can be caused by various causes, including trauma to the nail. Although it does not cause pain, onycholysis is uncomfortable and can last for months. However, it will generally heal on its own once the affected portion of the nail grows out. The average growth time for fingernails is four to six months and eight to 12 months for toenails.
The nail can become permanently detached from the nail bed in severe cases. If the condition is left untreated for a long time, it may even lead to a permanent change in the nail bed. If not appropriately treated, the nail will continue to turn yellow until it grows out on its own. As with any condition, treating the cause of onycholysis is crucial in restoring the pin to normal.
Fungal infection
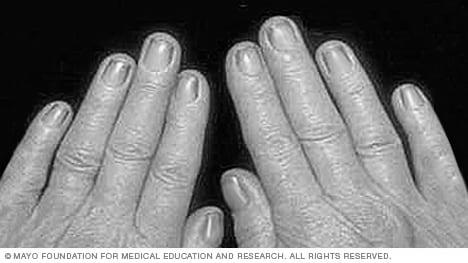
If your fingernails turn yellow, they may have a fungal infection. You can use oral medication or apply a medicated cream to your fingernails to fight the disease. However, this treatment can negatively impact the liver and interfere with other drugs. You should consider using an alternative therapy instead. Topical medications are usually more effective than oral ones, but they take some time to work.
Onychomycosis is a fungal infection of the nails caused by the fungus dermatophytes. The fungus thrives on keratin, a substance found in the skin and nails. About ten percent of adults develop this condition, and the risk increases as you get older. The fungus often attacks the feet of people with poor blood circulation, so you should be especially careful if you suffer from any foot disorders.
While the symptoms of yellow fingernails are temporary, it is essential to visit a doctor if they notice this condition on your fingernails. In many cases, the state is the result of a fungal infection. The situation can make walking painful and can even cause nail deformity. A doctor can also test for a bacterial or fungus infection and prescribe a more potent treatment.
The most common treatment for nail fungus is treatment. The nail fungus symptoms usually include yellow, thickened, or deformed fingernails. While this infection is generally less common in fingernails, it may also occur on toenails. People with diabetes, blood circulation problems, and weakened immune systems are more likely to develop nail fungus. However, this infection can affect anyone of any age.
Inherited condition
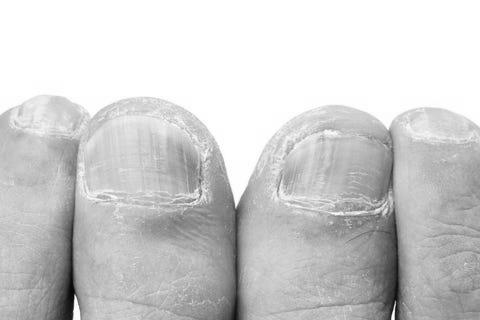
Inherited fingernail syndrome is a rare, inherited condition with symptoms ranging from thickened, yellow fingernails to respiratory manifestations. Although the exact cause of yellow nails is unknown, some reports in the medical literature have linked the condition to a mutation in the FOXC2 gene, a known cause of lymphedema. However, other studies have suggested that yellow nails are often misdiagnosed as asymptomatic.
Symptoms of yellow fingernails vary from person to person. In 85% of cases, the nail becomes thick and yellow, with some patients noticing their nails stop growing altogether. Even though the disease is rare, it has been reported to affect 1 in every million people. In men and women worldwide, it affects the fingers and toes equally. The condition may also affect newborns and young children.
Patients with yellow nail syndrome should visit a doctor if their fingernails have become discolored. Other symptoms associated with the condition include chronic sinusitis, cough, and pleural effusions. In 30% of cases, lymphocytes are detected. Some patients also develop lymphedema in the upper and lower extremities. If the symptoms are accompanied by an underlying respiratory problem, yellow fingernails may indicate yellow nail syndrome.
Inheritance of yellow fingernails is rare, but it can occur in people of all ages. Patients with yellow nails are usually older and have a history of respiratory or pulmonary symptoms. It is also believed that some titanium exposure has caused yellow fingernails. Some of the symptoms of yellow nail syndrome may also be triggered by a faulty immune system. Patients with the syndrome need to consult with a qualified physician as it is essential to determine whether it is related to a specific condition.
Genetics

There is a link between genetics and yellow nails. Researchers have identified a mutation in the FOXC2 gene that causes yellow nails. The conversion was previously associated with lymphedema-distichiasis syndrome. But some researchers think that the yellow nail syndrome is not an independent entity. In this case, the genetic defect may be the only cause of yellow nails. Genetics causes fingernails to turn yellow, and the condition may not be hereditary.
The exact cause of yellow fingernails is not fully known, but some theories point to the presence of genetics. A mutation in the FOXC2 gene may be associated with this condition, but further research is necessary. The transformation in the FOXC2 gene may cause yellow nail syndrome, although other literature reports that there is no genetic component. This condition is characterized by under-drainage of lymph fluid, which turns nails yellow.
Although yellow fingernails can signal underlying illnesses, genetics is not the only cause. Other diseases, such as arsenic poisoning, can also result in discolored fingernails. If the yellowing of your fingernails is caused by a fungus or a genetic disorder, you should consult a doctor. Your doctor should also check for any other symptoms that may be present. These could include breathing problems, leg swelling, and hair loss.
Research into the cause of yellow fingernails has uncovered no conclusive answers. Although most cases are random and sporadic, some sources classify the yellow nail syndrome is a primarily genetic disorder. If you wonder if genetics has anything to do with it, here is some information to get you started. When it comes to yellow nails, genetics plays an important role. Research has shown that yellow nails run in families. Although there are no genetic tests to confirm this, some other symptoms may indicate a disease of the fingernails.
Treatment
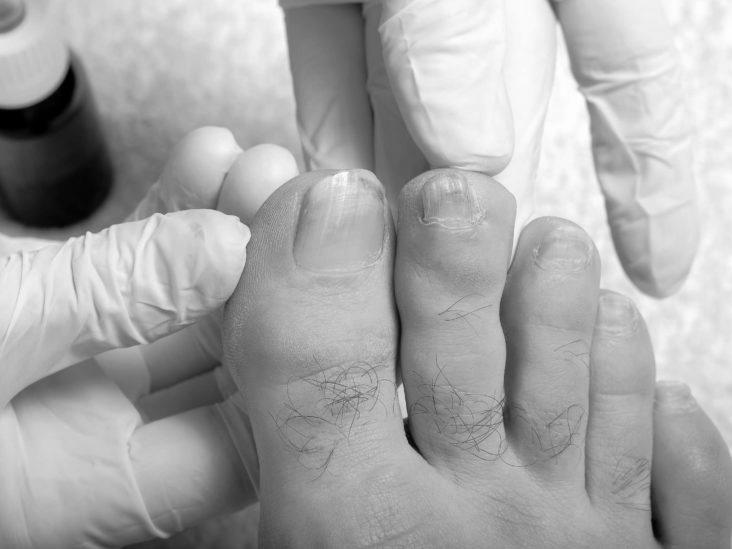
The best treatment for yellow fingernails depends on the cause of the problem. People who smoke are more likely to suffer from this condition. People with lung and liver diseases may also experience yellow fingernails. In some cases, yellow fingernails are caused by a disease called yellow nail syndrome. This condition affects the lymphatic system and the respiratory system and can result in thick, crumbling, or splitting nails. Treatment for yellow fingernails may require prescription medication.
Patients may also experience swelling in the arms and legs. In some cases, lymph fluid collects in the hands and legs. The swelling leads to reduced flexibility of the wrists, ankles, and nails.
The best treatment for yellow fingernails starts with prevention. You should avoid applying dark-colored nail polish to your nails, worsening the problem. Instead, use a lighter shade of nail polish. Also, apply a protective base coat to your fingernails to avoid staining. However, these measures only work temporarily. You should prevent acetone nail polish removers unless the condition is severe.
Other treatments for yellow fingernails include oral terbinafine or topical minoxidil. These are both effective and relatively inexpensive. They may also cause edema, but they may only treat the symptoms rather than the underlying disease. If you are worried about your nails, consult your doctor for more information. You should also visit a dermatologist if you have persistent yellow nails. They can prescribe antibiotics to help you manage the symptoms.
What Our Fingernails Don’t Tell Us About Our Health
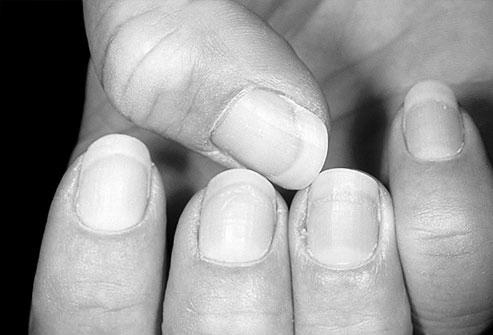
Did you know that our fingernails can tell us a lot about our health? This article will look at Yellow nails, Brown pigmentation, Mees’ lines, and vertical ridges. In addition, we’ll cover other common issues, such as aging. Hopefully, our fingernails will tell us more about our health than possible! But there are some conditions that our nails may not indicate, so keep reading!
Yellow nails

Our nails can reveal a lot about our overall health. Yellowing, discoloration, and lifted and crumbling nails can all indicate various health conditions, from pneumonia to heart failure. However, if we notice yellowing, we should not assume this is a medical condition. In fact, our nails can actually stain white, thanks to nail polish and acetone nail polish remover. These stains are standard but are not harmful to the health of the nail.
In some cases, we can see this condition in our nails because we are malnourished. In this case, the yellow color comes from an accumulation of debris underneath the nail. Your doctor may recommend a specialized treatment to treat your fungus. Various topical and prescription antifungal medications are available for this condition. This disease is also called onycholysis, a condition where the nail splits from the nail bed.
The antifungal properties of oregano oil make it an excellent treatment for yellow nails. This oil works well as a topical solution for nail discoloration. It is very effective and helps the nails grow. Apply the oil topically to the affected nails, and you’ll see a significant difference in your nails. Vitamin E has been used as a treatment for yellow nails for centuries. Aside from addressing the fungus, it can also treat the underlying cause of your yellowing.
Brown pigmentation

Some people believe that a black or brown streak on their fingernails indicates a disease, but this is not the case. In fact, it may be a sign of an undiagnosed medical condition. These streaks are part of the nail matrix beneath the fold, so they are challenging to see. If you notice such a condition, it’s best to seek medical attention as soon as possible.
Occasionally, a dark streak on a fingernail could signify melanoma, the deadliest form of skin cancer. Melanoma can develop on the fingernail or surrounding it and usually have no other symptoms. Often, the only thing that a patient will notice is the color of their fingernail. If you notice a dark streak on your fingernail, you should see a doctor immediately.
Other causes of brown pigmentation on fingernails include nail fungus. The fungus can cause fingernails to turn yellow or brown and, in severe cases, can cause them to crack or peel. Another cause of dark spots on fingernails is thyroid disease. It may be inherited or run in families. Treatment for this condition usually involves oral antifungal medication. Dark streaks under the fingernail can also signify melanoma, bruising, chronic infections, or drugs.
Mees’ lines

Mees’ lines, also called true leukonychia, are white bands that appear on the fingernails. These streaks can span the entire nail bed or be present on a single digit. Mees lines are typically associated with arsenic poisoning but can also be caused by radiation therapy, chemotherapy, leprosy, and certain toxins.
Mees’ lines can also indicate systemic stressors, such as heart failure and congestive heart failure. They’re also associated with infection and cancer. A 47-year-old Spanish man developed thick, white bands in the center of his fingernails 45 days after taking the Covid. According to the study’s authors, these wide white bands had never been observed before. Similarly, several patients have reported developing subtle ridges on their nails, referred to as beau lines.
Mees’ lines on our fingernails are a retrospective indicator of various diseases. These ridges form because of a temporary interruption of nail growth. This could be caused by physical stress, such as infection, malnutrition, and medication side effects. Beau’s lines are typically harmless but may become more noticeable over time. Symptoms of COVID 19 may include Beau’s lines.
Vertical ridges

Beau’s lines or vertical ridges on our fingernails often indicate underlying health conditions. They may also indicate a condition called psoriasis. These ridges may be caused by anemia, malnutrition, heart attack, and severe infections or can be a sign of poorly controlled diabetes. Fortunately, these lines typically clear up with time. Read on for more information on the causes of these ridges on fingernails they mean for our overall health.
In addition to being an aesthetically pleasing feature, ridges in our fingernails can also indicate underlying health conditions. These ridges may be a sign of diabetes, cardiovascular problems, or rheumatoid arthritis. Additionally, a single ridge in the middle of the fingernail could indicate a vitamin or nutrient deficiency. Here are the most common conditions that may cause vertical ridges on fingernails:
Fingernail ridges are tiny raised areas found on the nail’s surface that run from the cuticle to the tip of the nail. While they are considered a normal part of aging, they can also be a sign of underlying health conditions such as rheumatoid arthritis, anemia, and peripheral vascular disease. However, if you have raised ridges on your fingernails, you should seek medical attention as soon as possible.
Splinter hemorrhages

If you have a splinter hemorrhage in a fingernail, you may be wondering if there’s something wrong. These bleeds are actually bleeding from tiny capillaries under your fingernails. These will fade and grow out with the nail, so you cannot worry. But it’s still good to find out what’s going on!
If you’ve ever experienced a splinter in a fingernail, you know how uncomfortable they can be. These tiny splinters appear as longitudinal streaks beneath your fingernail, resulting from a ruptured blood vessel underneath your fingernail. They are often caused by trauma, although other diseases of the fingernail or blood vessels can cause them as well.
In addition to these splinter hemorrhages, a black line under your fingernail may indicate a more significant problem. While splinter hemorrhages are not dangerous, you should always see your doctor if you notice one. It’s important to know that a splinter hemorrhage can signify a more serious medical condition, so it’s worth visiting your doctor to get checked out as soon as possible.
In both cases, high glucose levels in the blood can damage the blood vessels and cause splinter hemorrhages. When it’s the cause of these blemishes, the best course of action is to consult your doctor.
Raynaud’s
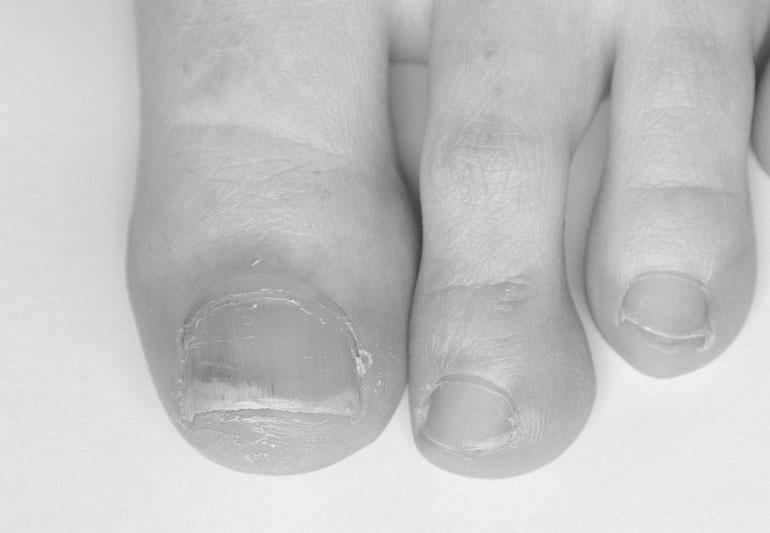
We’re familiar with the white or blue fingernails that indicate a potential health problem. However, you may not know that other symptoms mean this disease, including numbness, tingling, and burning. The condition can be caused by minor temperature changes, such as exposure to cold temperatures or stress. A doctor can help you determine the cause of your symptoms and prescribe the proper treatment.
When we’re experiencing symptoms of Raynaud’s disease, we’ll notice a white or blue coloration of our fingernails. The affected areas may also be red and throbbing, and they may even become so inflamed that they develop ulcers. Sometimes, they become so painful that the affected area can become gangrene. In these rare cases, the affected area may require amputation. Fortunately, several treatments for this condition can reduce the symptoms and help you maintain a healthy lifestyle.
Symptoms of Raynaud’s syndrome can be prevented by identifying triggers and avoiding cold environments. If your symptoms persist or get worse, you should seek medical care. It’s important to remember that cold climates can trigger Raynaud’s, but some people may have this condition without a temperature drop. Nonetheless, you should listen to your body’s signals.