How to Get Rid of Orange Fingernails
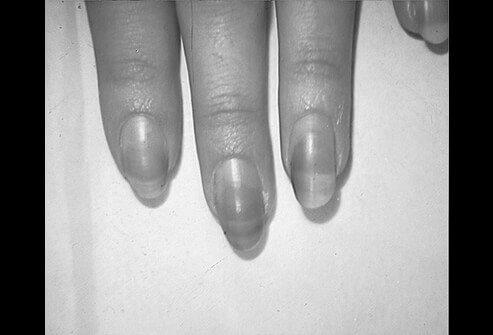
If you want to get rid of orange fingernails, you must avoid certain foods. Avoid eating oranges and peeling them. Soak your fingernails in warm water for 5 minutes every week. Also, avoid removing the cuticles. Finally, avoid using nail polish regularly. Drink enough water and eat a healthy diet. These tips can help you get rid of this problem and make your nails look great!
COVID-19

Orange fingernails are a symptom of COVID-19, a coronavirus. It causes an interruption of the matrix for the nails. Symptoms of COVID-19 include orange fingernails and transverse grooves in the nail plate. Patients may also have spoon-shaped nails, which are signs of hemochromatosis and anemia. Nevertheless, these symptoms aren’t necessarily signs of infection or a severe ailment.
Patients with COVID-19 infection have a high risk of developing onychomadesis, an infection of all toenails caused by the virus. The disease has also been associated with chilblain-like lesions. However, the exact cause is unknown. This condition is usually mild or sporadic, and a patient can develop both red and orange fingernails with the same virus.
In a recent study, British epidemiologist Tim Spector and colleagues identified a new symptom of COVID-related nail infection called “Covid nails.” This symptom appears as a red half-moon at the base of the fingernails. This new symptom presents earlier than other Covid-related nail complaints. The pattern is a red half-moon pattern formed over a white region at the base of the fingernails. This unusual appearance is sporadic, and there are no documented cases of Covid nails in people who have not suffered from it.
The symptoms of COVID-19 infection include a low blood oxygen level, which affects blood oxygen levels. However, COVID infection does not necessarily affect the blood oxygen level, but it can cause symptoms of various health issues, including mental well-being. Patients with COVID are encouraged to seek medical attention to ensure that the virus is not affecting their nails. The symptoms of COVID can show themselves through the pins, earlobes, and skin.
A few other symptoms of COVID include a red nail bed and a red or purple toe. This condition is often accompanied by other symptoms such as leukonychia, leading to severe COVID. It also can cause cyanosis, a condition in which the red blood cells can’t carry enough oxygen to the rest of the body.
Onychomycosis

Onychomycosis is an inflammatory condition that affects the nail bed. It is caused by several organisms, the most common dermatophytes of the genus Trichophyton. The infection can also affect the fingernails and may be mistaken for Psoriasis. It manifests as an intense inflammatory infiltration in the nail matrix. The overlying nail plate becomes detachable, and the infection occurs.
If you are concerned about your nail color and feel that it may be caused by a fungus, you should consult a physician. Treatment for onychomycosis is a combination of medical treatments and home remedies. There is no definite cure for this condition, and doctors will treat you based on your symptoms and suspected cause. If your symptoms are painful and you do not want to live with a disfiguring nail color, you can use oral antifungal medication to treat the condition.
Onychomycosis occurs on the nail plate in several different patterns, each with distinct symptoms. The two most common types are superficial and distal subungual onychomycosis. A distal lateral subungual form causes the nail plate to appear layered and can erode and split. A severely eroded nail may develop cracks and flaking. The endonym pattern of onychomycosis affects the entire nail matrix, and nails are often thick and lamellar.
Diagnosis of onychomycosis is based on a patient’s history, physical examination, and diagnostic studies. In a typical case, a diagnosis will include a dermatophytosis, a compact ball of fungal filaments that appears as a longitudinal streak on the nail plate. Occasionally, the disease can progress to the subungual layer of the nail plate, worsening the disorder and possibly partial loss of the nail plate.
The condition can also cause yellow or white patches under the nail tip. A whitish patch near the cuticle is indicative of a form of proximal subungual onychomycosis, which is most common in people with compromised immune systems. This infection is also a sign of HIV. A white patch on the toenail can also indicate a fungal infection.
Paronychia

Yellow or orange fingernails can signify various conditions, including fungal infection or bacterial infection. Fungal infections can cause your fingernails to thicken and crumble. In some cases, yellow or orange fingernails can also indicate that your body isn’t getting enough oxygen or may be suffering from a bacterial infection. In some instances, bluish fingernails can indicate lung disease, such as emphysema, while pitted or rippled nails may indicate Psoriasis. Inflammatory arthritis can also cause discoloration, and the skin underneath can be red.
Some people experience orange fingernails due to a vitamin deficiency. Another common cause is eating too many carrots or sweet potatoes. Occasionally, orange fingernails may be a sign of a fungal infection and should be treated by a doctor. If orange fingernails are persistent, they may need to be removed or replaced. Always eat a well-balanced diet and drink enough water to avoid further health problems.
Another cause of orange fingernails is malnutrition. Undernutrition can cause the discoloration of the fingernails, and it may take several weeks or months before the disorder is ultimately manifested. Fat-soluble vitamin deficiencies can take more than a year to manifest themselves. You may need to take supplemental vitamins if you notice discoloration. B baking soda water may be beneficial for those who don’t have a vitamin deficiency.
Other causes of discolored nails include trauma to the skin or nails. Trauma to the skin can make it more conducive to fungal infection. It may spread to other fingers, so you should keep your nails clean. To prevent this, clean your nail clippers and wear new shoes and socks. It’s also important to wash your boots because some spores can remain viable for several months in a shoe or socks.
Moreover, orange discoloration on the fingernails is a severe symptom of chronic renal failure. In one case, an elderly patient, who had been diagnosed with COVID-19, developed discolorations on her fingernails 16 weeks after the outbreak. During the illness, the woman also developed anemia. The lesions did not improve when the patient was examined a month later.
Lack of hydrochloric acid

A lack of hydrochloric acid is a leading cause of orange fingernails. In addition to discoloration, the condition can be a symptom of other diseases, including high fever, arsenic poisoning, and heart disease. In rare cases, a lack of this acid may also cause fungus to grow on nails or around the nail. It can also result in the splitting of the nails. While the symptoms listed above do not necessarily mean a diagnosis, they indicate that you should visit a physician. For example, if you notice white spots on your nails or white lines running parallel to the lunula, this is a sign of kidney or liver disease, or if you see dark areas around the nail bed, you could have a systemic illness.
Researchers have found that the lack of hydrochloric acid is associated with many other diseases, including bacterial dysbiosis and iron deficiency. Despite these findings, a lack of hydrochloric acid can cause a nail abnormality. However, treatment for the condition is expensive, and some people may require more than one treatment. However, the long-term benefits are well worth it.
Many factors can contribute to low stomach acid production. In addition to improper diet, a vitamin deficiency may also cause this problem. Stress and excessive alcohol consumption can deplete a person’s stomach acid, leading to various chronic health problems. If the pain is severe, your doctor may refer you to a gastroenterologist for further testing. If you’re concerned about the symptoms of hypochlorhydria, consult a medical professional to see if they can prescribe a treatment that can correct the problem.
Occupational exposure to arsenic, thallium, or mercury can cause discoloration of the nails. However, the cause is often unknown. Mees’ lines usually indicate heavy metal poisoning and generally grow out of the pin. A case-controlled study by Shafiquzzaman et al. failed to show a significant association between Mees’ Lines and arsenic levels in the nails. Some other potential causes for this condition include chemotherapy and renal failure.
Why Do Doctors Push on Your Fingernails?
Why do doctors push on your fingernail? These changes are regular and can point to an underlying health condition. If you’re worried, it’s good to discuss the issue with your doctor. You can find out if the change is related to thyroid disease or Psoriasis. And if the change isn’t related to a medical condition, you can also ask your doctor for a second opinion.
Inflammation of the nailbed
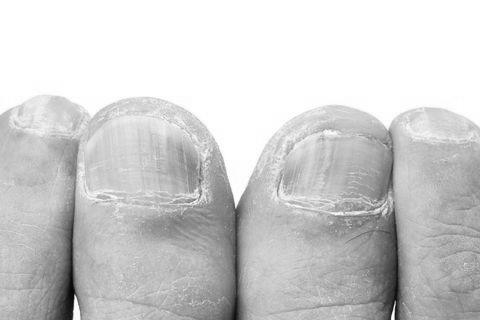
Inflammation of the nailbed when doctors press on your fingernails is often mild and can resolve independently. However, it can be severe enough to require medical treatment in more severe cases. Antibiotics, such as Keflex or Bactrim, can be prescribed. A physician may also elevate the hardened skin bordering the nail to drain the pus. This is similar to draining an abscess.
When physicians push on your fingernails, they may also lift the nail plate. This is a common side effect of certain medications, including chemotherapy. Although it is usually temporary, it can be uncomfortable and increase the risk of infection. Another side effect of certain medicines is different-looking ridges or colored lines on the nail plate. While these changes are usually temporary, they are an indication that the problem has been diagnosed.
Inflammation of the nail bed may be a symptom of a bacterial infection or a more severe problem. The nail bed may be inflamed, and the skin underneath may be infected. Medications or radiation treatments can also cause nail color changes. Sometimes, the resulting discoloration is due to a bacterial or fungal infection. In either case, the inflammation is painful and may limit a person’s activities.
A doctor may diagnose you with Paronychia, an infection of the folds of skin surrounding the fingernail. The disease can be acute or chronic. During acute paronychia, trauma to the folds causes pathogens to invade the nail. Treatment options include corticosteroid-based topical antibiotics and warm compresses. In severe cases, surgical incision and drainage may be necessary. However, in chronic Paronychia, the infection can cause more severe complications, such as abscess formation or an abscess.
Paronychia is a painful inflammation of the nailbed that usually develops after an injury to the nail. This is a result of bacteria. It can also be caused by overly aggressive nail care, such as over-biting the fingernails or damaging the skin surrounding them. The infection can spread throughout the body, resulting in a white, flaky nail bed.
Signs of Psoriasis

Your doctor might not know your symptoms, but these changes in your fingernails could mean several things. Some people experience discoloration, brittleness, or even crumbling of their fingernails. These changes can also indicate an infection beneath your fingernail or an autoimmune disease known as Psoriasis. If your doctor pushes on your fingernails, ask them to examine the surrounding area.
If you’re worried about the appearance of these symptoms, you should talk to your doctor as soon as possible. The first symptom of Psoriasis is the appearance of yellow, flaky skin on your fingernails and toenails. This condition can also cause the nail to peel or break, leaving you without a single pin.
A doctor may push on your fingernails and recommend you visit a dermatologist. Your doctor might recommend that you wear gloves to prevent any infections. Wearing vinyl gloves won’t give you the necessary protection. Keeping your nails clean and dry will also reduce the risk of disease. Don’t wear fancy fingernails, as this could irritate your nails.
Psoriasis is a chronic condition of the skin. People with the disease develop red patches covered in silvery scales that can appear anywhere on the body. The skin is sore and itchy, and the condition can affect any joint, including the fingernails. A doctor can recommend treatment options or give you lifestyle tips and guidance to help you cope with flare-ups.
You can take corticosteroid injections for Psoriasis, but these don’t work for everyone. Instead, doctors may prescribe oral medications that target the underlying inflammation. They are very effective in treating Psoriasis, but they can come with side effects. Fortunately, some treatments are safer and more effective than others.
Keeping your nails short can help prevent infections and reduce the risk of crumbling or breaking. Also, wearing cotton gloves when working in water can help prevent nail damage from scratching. And you shouldn’t pick your fingernails or use sharp objects to clean them. Alcohol is another trigger. While it doesn’t seem like it should be a trigger for Psoriasis, alcohol can worsen your symptoms.
Signs of thyroid disease

Hypothyroidism can show up in many ways, including on your nails. If your nails are split or crumbled, this may signify hypothyroidism. Other symptoms may be unexplained weight gain and fatigue. A blood test can reveal if you have this disease. Treatment options for this condition can range from vitamins and supplements to surgery. Often, doctors recommend lifestyle changes along with prescription thyroid medication.
Muscle aches and muscle breakdown may be a sign of an underactive thyroid. The muscles in your neck are the first to develop symptoms of thyroid disease. Swallowing problems and difficulty swallowing can also be signs. Thyroid testing is an essential checkpoint in your healthcare routine. But what if the symptoms are not so apparent? You may not be able to tell if you’re suffering from a thyroid disorder until it becomes too late.
White spots on your fingernails may also signify selenium deficiency or undiagnosed thyroid disease. The white spots can be caused by an overactive thyroid, allowing the fungus to penetrate beneath the nail. Fortunately, a proper diagnosis can prevent the fungal infection from spreading. If you’re concerned, consider taking an antifungal medication to fight the fungus before it even gets a chance to spread. Keep your feet dry and clean to prevent the growth of fungal infections.
You can feel tired and sluggish when you have an overactive thyroid. You may be irritable and experience frequent bathroom visits. You may also experience prolonged confusion. In addition to low or overactive thyroid, you may feel cold or have trouble waking up in the morning. Your heart may feel weak or heavy, and you may be prone to anxiety and depression.
If you’re concerned that your thyroid might be overactive, your doctor may use a thermometer to test your blood. A temperature increase may be another sign. This condition may also cause you to be extra sensitive to heat, and you may tend to sweat all the time. Diabetic patients are more likely to develop complications from thyroid disease, as hyperthyroidism increases insulin resistance, which is bad news for diabetics.
Signs of a hangnail
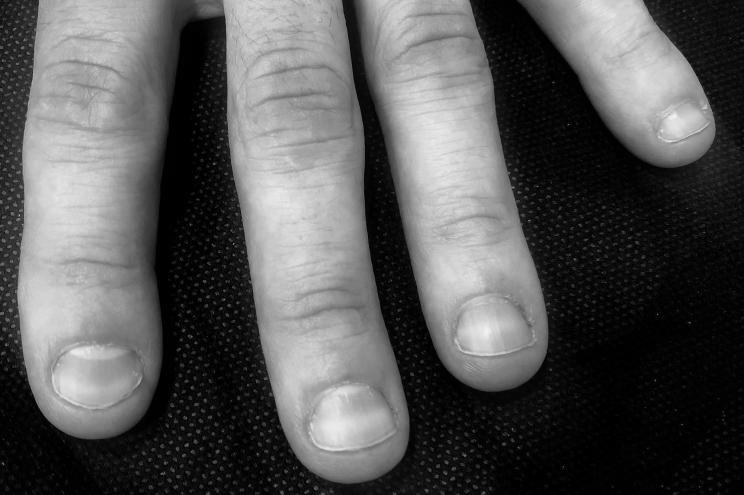
The first sign of a hangnail infection is redness, swelling, and tenderness in the affected nail. If the pin is infected, it may spread further down the finger or hand. In some cases, the infection can become chronic and result in a loss of sensation. If the condition is left untreated for 6 weeks or more, it can even lead to the amputation of the nail. Fortunately, home remedies can be very effective in mild cases of hangnail infection. However, severe cases of disease that cause pus may need medical attention.
If the hangnail becomes infected, a doctor may prescribe antibiotics or perform a drainage procedure. If the infection has not cleared up after a week, it is best to see a doctor for further testing. Hangnail treatment may include applying topical steroids or antibiotic cream. Surgical procedures may also be necessary if the infection is a fungus. However, most hangnails clear up on their own with no further complications.
A warm water soak is a good treatment for an inflamed hangnail. After the soak, you can apply antibiotic cream or moisturizer to reduce swelling and minimize the risk of further infection. While home treatments are effective, it is advisable to see a doctor if your hangnail has become infected because it can increase infection chances. So, what are the signs of a hangnail?
An infected hangnail is also called Paronychia or whitlow. It occurs when the nail plate grows into a fold or crease in the skin. While most cases of acutely infected hangnails are uncomplicated, infected hangnails can lead to severe pain and discomfort. Luckily, these infections are highly treatable. And even if they do not, the cure will be as simple as a visit to the doctor.
The signs of a hangnail should not be ignored! If left untreated, the condition could lead to an infection in the surrounding skin and spread elsewhere. It is essential to see a doctor if you notice pus in the nail fold or under the hangnail. Even if it doesn’t improve after a week, a doctor can still identify the infection by looking at the nail fold and using sterile nail clippers. When trimming a hangnail, make sure you do not cut too deep, as this can damage the nerves and tiny blood vessels in the skin underneath the hangnail.